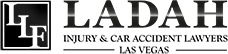Most people are unfamiliar with the purposes of cortisone injections. The general understanding is that they help alleviate pain in localized areas of the body such as in joints and sometimes in soft tissue as well. What isn’t well known is how these injections work.
As an injected steroid, cortisone injections function as an isolated anti-inflammatory drug giving lasting relief in the affected area. Relief of inflammation is how most OTC pain relievers work. They are typically called NSAID or Non-Steroid Anti-Inflammatory Drugs. The pain relievers you grew up with; aspirin, ibuprofen, acetaminophen, and naproxen are all anti-inflammatory drugs.
Most people pop an aspirin or other OTC pain reliever without giving it much thought. We have been conditioned to believe that they are safe; yet an estimated 7,600 deaths and 76,000 hospitalizations in the United States are the result of taking NSAID. The unspoken truth is that casual consumption of NSAID is dangerous and damages the liver and other tissues, particularly in the GI tract. However, the danger is often glossed over as reflected in the cursory statement, “Take 2 aspirin and call me in the morning.”
Cortisone injections are dangerous as well. They are a preferred treatment for local inflammation mainly because oral anti-inflammatory medication affects the whole body and not just the affected area. The potential damage to the injection area is significant, especially when overused. As useful as anti-inflammatory drugs can be, any overuse will cause damage.
Cortisone injection risks your doctor may be ignoring
Cortisone injections are similar to NSAID with respect to moderate occasional use; they can be beneficial, especially for people suffering from joint pain. But just like NSAID, some people shouldn’t flirt with anti-inflammatory drugs and long-term use will negatively affect most everyone.
Side effects may include weakened tendons; tendon ruptures, thinning of the cartilage, infection, and sometimes even increased inflammation due to a reaction to the drug. Doctors also need to consider when cortisone injections could be even more risky. The injection can significantly elevate the blood sugar in diabetic patients. Also if the patient has any infection, the shot hinders the body’s ability to fight it off. Consequently, cortisone injections should be used cautiously with diabetics and avoided altogether with any patient with an active infection.
Complications from long-term cortisone use can, among many other side effects, elevate blood pressure, cause cataract formation, thinning of the bones, and even avascular necrosis.
Conclusion
Cortisone injections in the hands of a cautious and conscientious doctor can be beneficial. However, doctors that indiscriminately administer cortisone as they would a bandaid, may be doing more harm than good.